Venous Specialists
Expert and Effective Care
The UK’s dedicated private clinic for the
treatment of circulatory and vascular disorders, especially problem veins
We are experts in disorders of the circulatory system including arteries, veins and lymphatics. We use the most up-to-date techniques and state of the art equipment to achieve the best possible results for circulatory problems.
radio frequency ablation
Endovenous Laser Ablation
Sclerotherapy
Phlebectomy
We are vascular experts who specialist in
vein problems
60 sec video
60 sec video
State of the art treatment for problem veins
Faulty veins can take many forms, from life threatening thromboses to cosmetic surface veins. We are vascular specialists and experts in circulatory disorders. We use the most up-to-date techniques and state of the art equipment to treat vein disorders of all kinds.
treatment options for varicose veins
Ian Franklin participates in a discussion about varicose veins on BBC Radio 4’s Women’s Hour with Jenni Murray and a patient.
8 min audio
book your appointment
Dedicated to providing the best possible results for vein disorders
The London Vascular Clinic team are all specialists in disorders of the circulation. Our background, training and long experience in general vascular surgery provide the foundation for our specialty focus today in treating disorders affecting the venous system.
before & after
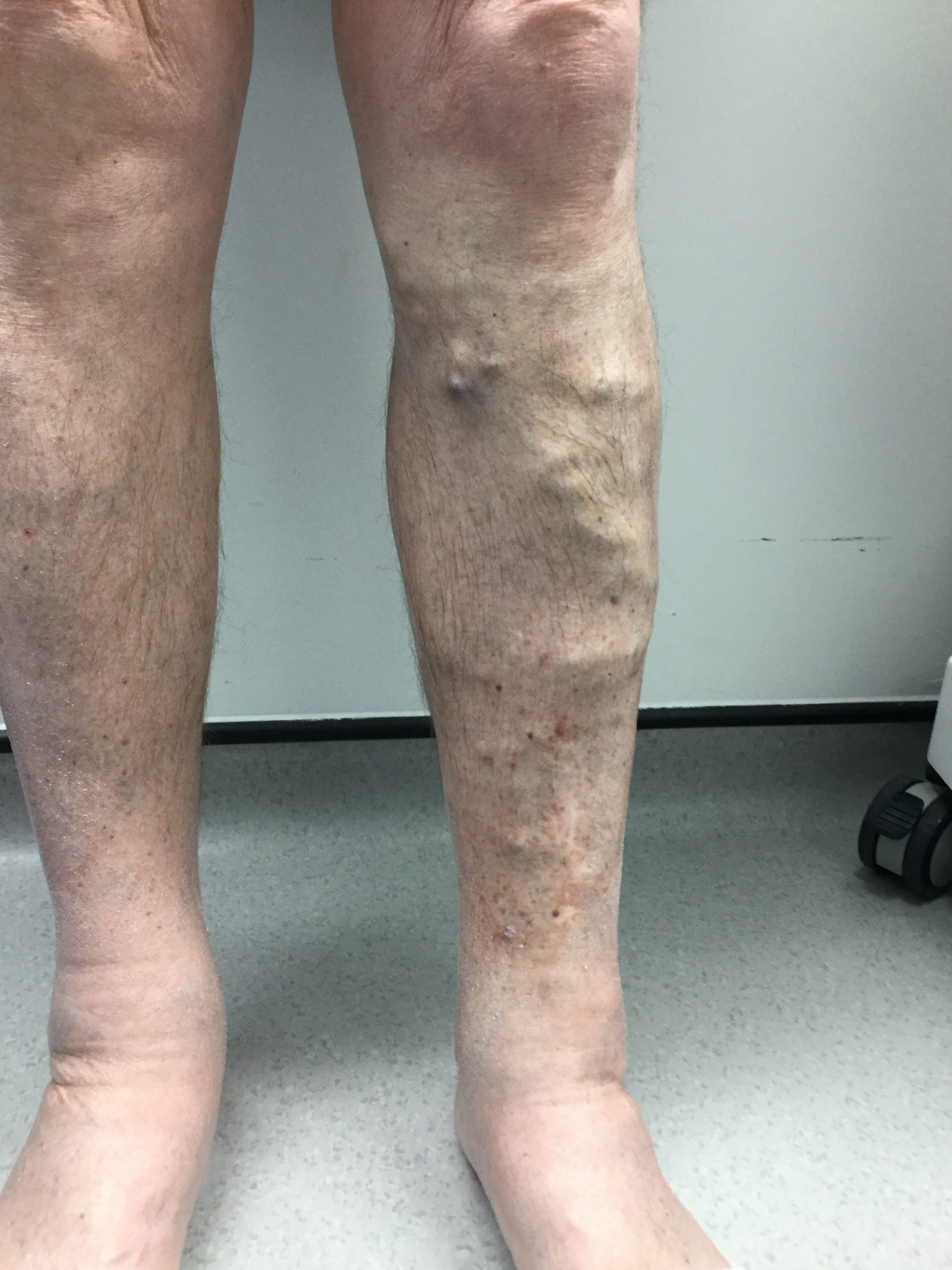
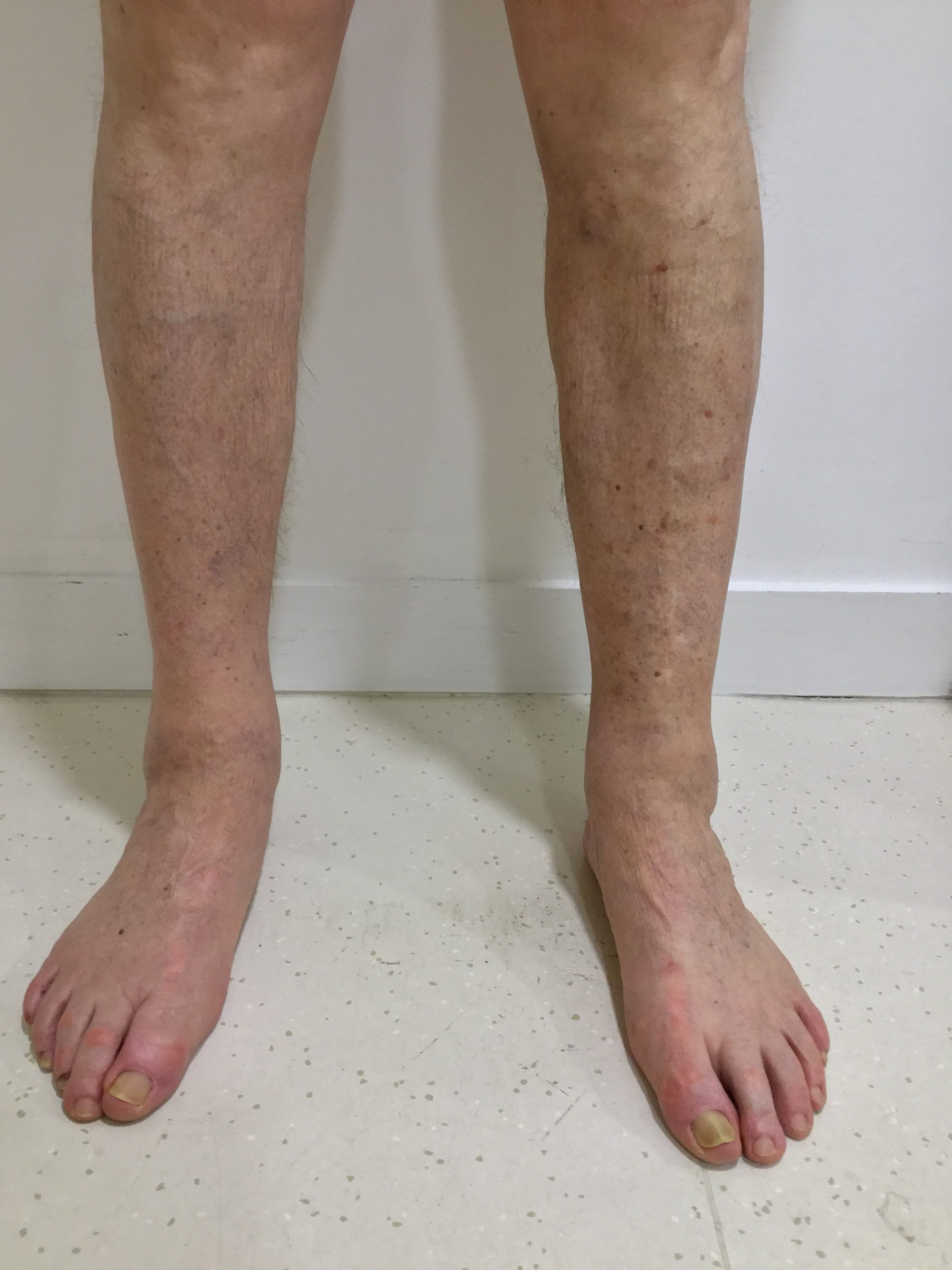
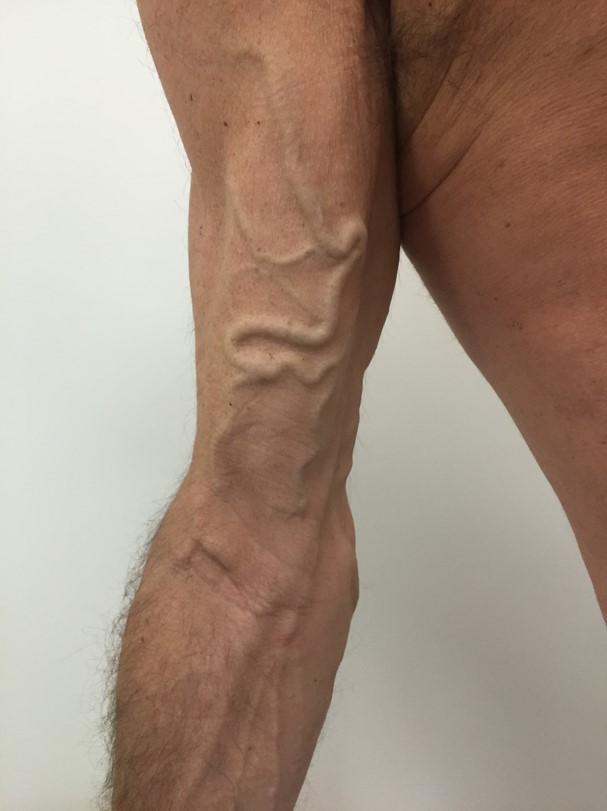
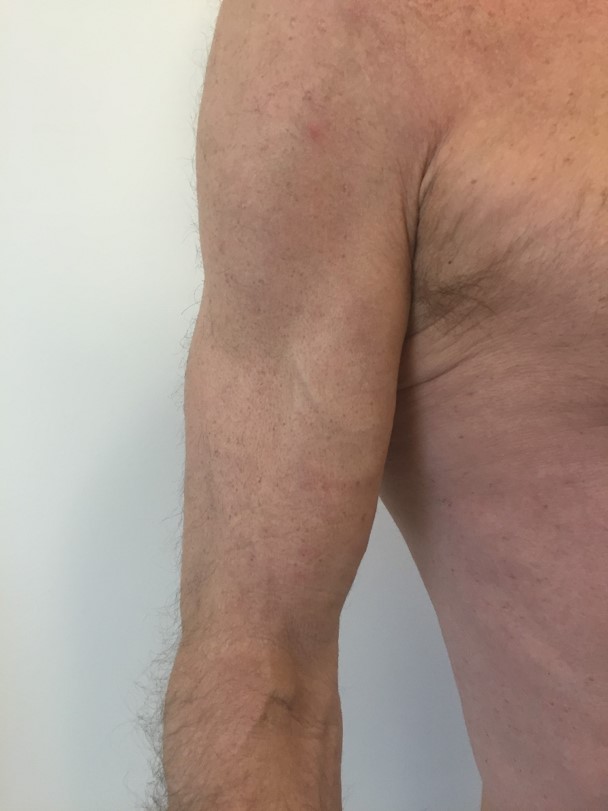
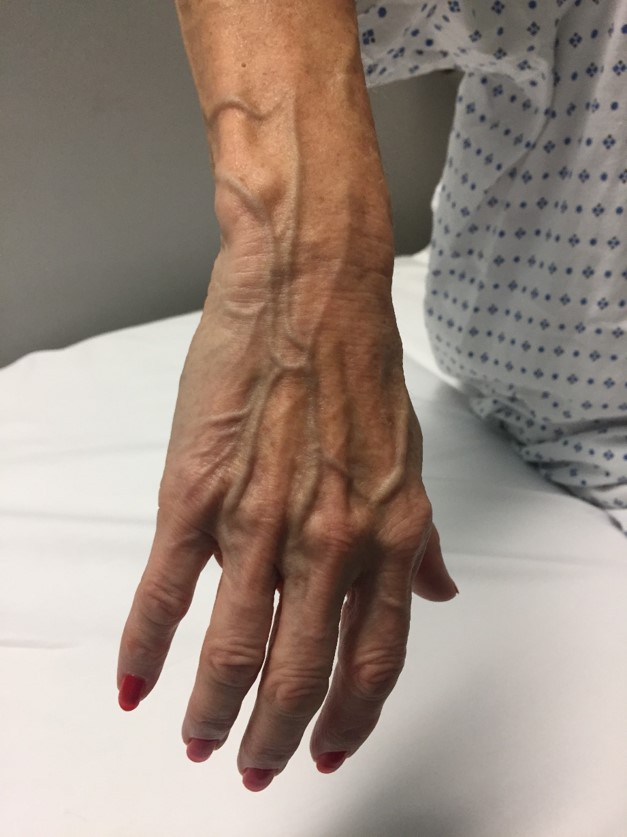
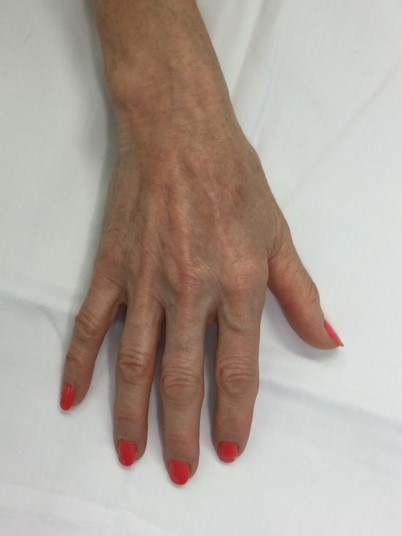
the vision
from the beginning
Ian Franklin is a senior and experienced vascular surgeon. In 2013, after 23 years of full time NHS service he became a full-time venous specialist. He now leads a team that dedicates itself to providing the best possible treatment for patients affected by venous problems of all kinds.


where we work
We are happy to see you at any of these top London hospitals.
Online consultations also available.

What People Say About Us
Client Testimonials



meet our
expert team
Mr Ian Franklin
Angela Williams
Hema Rao
How can we help you?
three steps to deal with your problem veins
01
Arranging your consultation
To book your appointment simply contact us by phone, email, Whatsapp or the contact form below. We offer consultations every weekday and you have a choice of three locations and morning, afternoon, and evening appointments. Circulatory problems usually require assessment with a duplex scan (doppler-ultrasound), a special from of ultrasound which provides detailed anatomical and functional information on blood vessels. We can provide this at the time of your first visit to see us. When you book our team will ask you some details of the problem so the appropriate scan can be scheduled for you.
02
The consultation
When you arrive, you will be greeted by the reception team and taken for your duplex scan by an experienced vascular scientist. This is completely painless. The scan is performed in a slightly darkened room with you standing on a special footstool next to the examination couch. As part of the process your calf muscle is squeezed to stimulate blood flow through your veins. The scan usually takes between 25-60 minutes depending on the complexity of the problem.
After the scan you will see Mr Franklin to discuss all your concerns and symptoms and have a physical examination. We will then analyse your scan and decide on the treatment options that are available to you. We allow plenty of time for discussion and will make sure all your questions are answered.
03
The treatment
The treatment you might require obviously depends on the nature of the problem. Some circulatory disorders require complex interventions. Others are more straightforward.
Treatment for superficial vein problems commonly takes two stages. First it is necessary to correct the main structural problem. The method chosen depends on the shape and size of the problem vein. This part of the treatment is often covered by private health insurance. Once the underlying structural problem is dealt with the surface cosmetic veins can be treated. This usually requires a combination of sclerotherapy and laser treatment to achieve the desired aesthetic result.